Live Hands-On CME Workshops
Hands-On Training. Fun and Interactive. CME for For Nurse Practitioners, Physician Assistants, and Physicians
Clinical Skills
and Procedures
Book Early and Save!
Airway, Suturing,
and Radiology
Book Early and Save! - ONE DATE ONLY
Ultrasound,
Skills and Procedures
Book Early and Save!
Our INTERACTIVE live programs give you supervised procedural performance and teach you decision-making under pressure
Airway, Skills
and Procedures
Book Early and Save!
Ultrasound and
Advanced Airway
Book Early and Save!
Advanced Airway and
Advanced Suturing
ONE WEEKEND ONLY! Book Early and Save!
The Clinical Skills & Procedure Workshop

2-Day Conference + Hands On Workshop
The Clinical Skills and Procedure Workshop is perfect for any provider in primary care, hospitalist, emergency, or urgent care.
Interactive, current, evidence-based presentations combined with hands on procedure workshops
23 Category I CME credits with additional credits for Emergency Procedures and Pharmacology
Program also includes a tote bag, full sized textbook with reference normal images and room for notes, coffee and beverage service throughout the day, and lunch.
Discounted hotel rooms are available.
A must-take program for anyone in clinical practice!
The Advanced & Difficult Airway Workshop

1-Day Hands On Workshop
A comprehensive hands on airway management procedure course combined with individual clinical scenarios
Taught by our expert faculty and combines real world experience with the latest evidence-based airway management techniques
Can be combined with our 2-Day Clinical Skills and Procedure Workshop
Limited availability.
Up to 33 Category I CME credits with additional credits for Emergency Procedures and Pharmacology
A must-take program for anyone in clinical practice
All programs also include a complimentary 1 year membership and subscription to our online Clinical Toolkit!
Discounted hotel rooms are available
Perfect for Nurse Practitioners, Physician Assistants, and Physicians.
The Ultrasound
Workshop
Workshop

1- Day Hands On Workshop
High quality and detailed presentations from our expert faculty
Hands on instruction with live models
Low student to instructor/model ratio ensures plenty of individual attention and free scanning time
Uses the latest wireless high resolution portable equipment
Can be combined with our 2-Day Clinical Skills and Procedure Workshop
Limited Availability.
Up to 37 Category I CME credits/Contact Hours with additional credits/hours for Emergency Procedures and Pharmacology
A must-take program for anyone in clinical practice!
All programs also include a complimentary 1 year membership and subscription to our online Clinical Toolkit!
Discounted hotel rooms are available
Designed for Nurse Practitioners, Physician Assistants, and Physicians
The Advanced Suturing Workshop

1-Day Hands On Workshop
In addition to our basic suturing course, knot tying, and common suture patterns
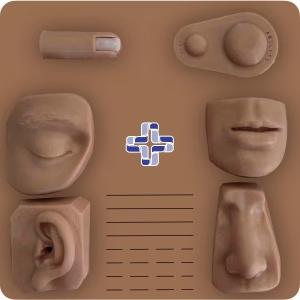
Focused instruction includes suturing of specialized body parts (ear, nose, lip, mouth, eyelid, and finger.) in addition to our basic suturing course, knot tying, and common suture patterns
Also includes nail trephination, abscess incision and drainage, and cyst removal
Hands-on instruction with low student to teach ration ensures individual attention and mastery
Can be combined with our other workshops
Limited Availability.
12 Category I CME credits/Contact Hours with additional credits/hours for Emergency Procedures and Pharmacology
Workshop includes our own customized suture simulator, individual instruments, and materials.
All programs also include a complimentary 1 year membership and subscription to our online Clinical Toolkit!
Discounted hotel rooms are available
The Advanced Suturing Workshop
Learn how to approach complex laceration management and get hands-on training on our custom simulator. Includes Ear, Nose, Lip, Eye, and more

NP/PA Credit
This activity has been reviewed by the American Academy of Physician Associates Review Panel and is compliant with AAPA CME Criteria. This activity is designated for 100 AAPA Category 1 CME credits. PAs should only claim credit commensurate with the extent of their participation. Approval is valid from 2/20/2026 to 2/19/2027. AAPA reference number: CME-2014150.

The AAFP has reviewed the Physician Skills and Procedures Series, and deemed it acceptable for AAFP credit. Term of approval is from 05/01/2026 to 04/30/2027. Physicians should claim only the credit commensurate with the extent of their participation in the activity.
Spring Break Sale!
TAKE 20% OFF
ANY LIVE program in March, April, or May!
Discount taken automatically. Offer ends March 8, 2026. Act now!

Upcoming Dates
Upcoming Dates

-
Sale!

2-Day Advanced Airway and Suturing CME Workshop – July – Dallas, Texas
$1,895.00Original price was: $1,895.00.$1,695.00Current price is: $1,695.00. Add to cart -
Sale!

1-Day Advanced and Difficult Airway CME Course – August – Washington, DC
$1,095.00Original price was: $1,095.00.$995.00Current price is: $995.00. Add to cart -
Sale!

2-Day Advanced Suturing and Airway CME Workshop – October – Orlando, Florida
$1,895.00Original price was: $1,895.00.$1,695.00Current price is: $1,695.00. Add to cart -
Sale!

2-Day Advanced Suturing and Airway CME Workshop – August – Orlando, Florida
$1,895.00Original price was: $1,895.00.$1,695.00Current price is: $1,695.00. Add to cart -
Sale!

1-Day Advanced and Difficult Airway CME Course – October – Orlando, Florida
$1,095.00Original price was: $1,095.00.$995.00Current price is: $995.00. Add to cart -
Sale!

1-Day Advanced and Difficult Airway CME Course – August – Orlando, Florida
$1,095.00Original price was: $1,095.00.$995.00Current price is: $995.00. Add to cart -
Sale!

1-Day Advanced and Difficult Airway CME Course – September – Dallas, Texas
$1,095.00Original price was: $1,095.00.$995.00Current price is: $995.00. Add to cart -
Sale!

1-Day Advanced and Difficult Airway CME Course – July – Dallas, Texas
$1,095.00Original price was: $1,095.00.$995.00Current price is: $995.00. Add to cart -
Sale!

1-Day Advanced and Difficult Airway Course – May – Dallas, Texas
$1,095.00Original price was: $1,095.00.$995.00Current price is: $995.00. Add to cart

Upcoming Dates
Maximize your time with small group, high yield, interactive educational sessions over 1, 2, or 3 days. Have fun in a small setting with high fidelity simulators!
Workshops can be taken by themselves or bundled with others for maximum flexibility.