Lindsay Portz, PA-C
Knowing how to diagnose Deep Venous Thrombosis (DVT) and choosing optimal treatment recommendations is a crucial skill in both the inpatient and outpatient settings. Virchow’s triad of stasis, hypercoagulability, and endothelial injury is the classic triad that causes clot formation.
Venous Stasis
Immobility of the lower extremities causes blood stasis. Blood usually will pool in the calf veins when a patient is supine. You can prevent venous stasis in your patients with elevation and/or mechanical compression of the lower extremities. Pharmacologic prophylaxis and post-op early ambulation may also prevent DVT after surgery.
Hypercoagulability
Inherited or acquired coagulation defects can increase DVT risks. Some of the inherited conditions are antithrombin III deficiency, deficiencies in protein C and S, Factor V leiden, hyperhomocysteinemia, and prothrombin gene 20210 mutation. Acquired hypercoagulability states can come from smoking, oral contraceptives/pregnancy, antiphospholipid syndrome/Hughes syndrome, malignancy, antineoplastic drugs (chemotherapeutic agents), and myeloproliferative syndromes.
Endothelial injury
Endothelial injury may occur during operations, applying prolonged compression on large veins, and indwelling venous catheters. It is important to distinguish between superficial thrombophlebitis and DVT when working up a patient because some of the symptoms shared between these two diagnoses may be similar. Also, deep venous thrombosis and superficial thrombophlebitis and DVT may occur together.
Superficial Thrombophlebitis Symptoms
Superficial venous cords can form in the upper or lower extremities. Patients have tenderness and erythema along the superficial veins. There is a preference to involve prior varicose veins, and symptoms may also include a low grade fever
Deep Venous Thromboembolism (DVT) Symptoms
Deep venous thrombosis usually presents with unilateral leg pain and symptoms. These symptoms include swelling, warmth, and tenderness of the extremity. It’s important to consider that upper extremity and bilateral extremity involvement also occurs. Malignancy is a risk factor for clot formation, so be on the lookout for signs of malignancy in your patients.
Phlegmasia Alba Dolens and Phlegmasia Cerulea Dolens
These conditions also present with dramatic leg swelling with white or bluish discoloration. They occur in patients with typical DVT risk factors. In rare circumstances a venous gangrene may occur.
Diagnosis of DVT
Physical Exam
Evaluate your patient for some of the signs and symptoms listed above. In addition to those signs and
symptoms, it is important to also evaluate your patient for pulmonary embolism (PE). Those signs and
symptoms may include tachycardia, dyspnea, pleuritic chest pain, cough, wheezing, hemoptysis,
syncope, or hemodynamic instability. Special tests to consider include looking for pain with passive dorsiflexion of the foot (Homan’s sign). Although classically associated with the diagnosis, it is not often apparent and it’s absence should not exclude DVT as a diagnosis.
Imaging/Labs
Ultrasonography
Duplex ultrasound is 90 to 100% sensitive for proximal femoropopliteal vein thrombosis or upper/proximal leg DVT. However, this is less sensitive in the calf for deep venous thrombosis. The rate of sensitivity in this location is 60-90%. You should order a follow-up study if ultrasound is equivocal. CT venography, MR venography or invasive venography are next-line studies.
D-Dimer and Wells’ Criteria
The d-dimer is a marker of fibrinolysis and also used as a screening test to rule out a DVT. You must determine a pretest probability using the Wells’ criteria to use this test effectively.
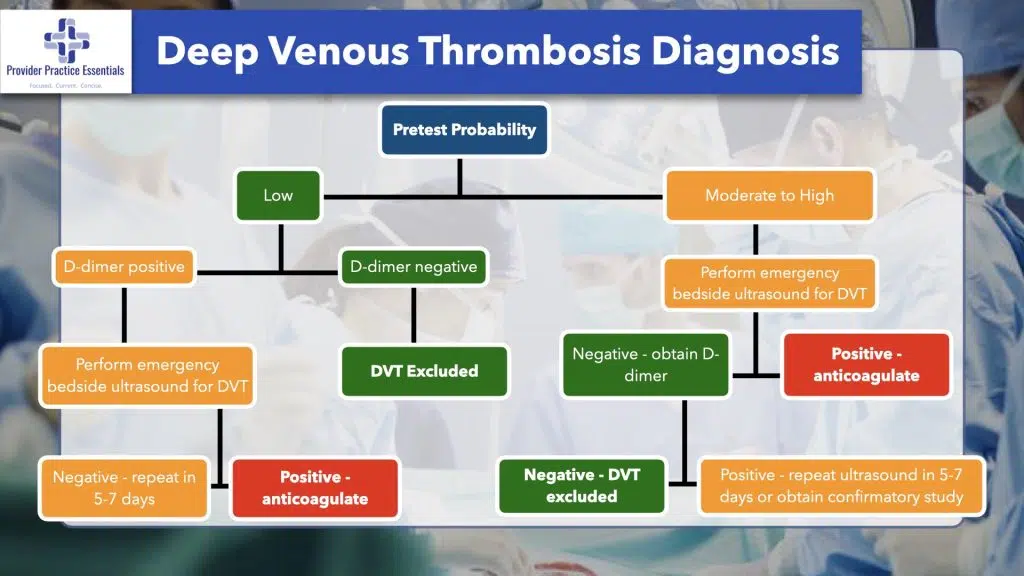
If your patient has a low probability and a negative d-dimer, the negative predictive value exceeds 99%, so you will not likely need to order an ultrasound. A positive D-dimer does not mean a patient has a DVT, but you should order an ultrasound to find out. Keep in mind many other diagnoses may show a positive d-dimer besides a DVT:
- Pregnancy
- Malignancy
- Recent surgery
- Immobility
Treatment of DVT
DVT should be managed with anticoagulation. There are circumstances where endovascular or surgical intervention is necessary. Recommended anticoagulation time is a minimum of 3 months. Patients with 2 or more episodes of DVT or high clotting risk factors should be anticoagulated indefinitely.
Novel oral anticoagulants (NOACs)
These medications have become the treatment of choice for uncomplicated DVT. They work quickly and do not require lab monitoring. However, these drugs are not the best for people with severe liver or renal dysfunction. The two most common drugs used in this category are Rivaroxaban (Xarelto) and Apixaban (Eliquis). For initial treatment of DVT with rivaroxaban (Xarelto), the patient needs to take 15 mg twice a day with food for the first 21 days. On day 22, change to 20 mg daily with food for the remaining treatment period.
For initial treatment of DVT with apixaban (Eliquis), the patient should take two 5 mg tablets twice a day for the first 7 days (4 tablets daily). After 7 days, reduce the dose to one 5 mg tablet twice a day until completion of treatment (2 tablets daily).
Heparin
Continuous heparin infusion can also be used to treat DVT. Treatment is completed with an IV bolus of 5000 to 10,000 units followed by a continuous infusion using a weight-based protocol of 1000-1500 units/hour. Activated partial thromboplastin time (aPTT) is used to monitor heparin in most hospitals. Monitoring should be at least 1.5 to 2.0 times pretreatment levels. It is very important to reach therapeutic levels within 24 hours. It’s also important to check platelet counts to recognize heparin-induced thrombocytopenia (HIT), and this will usually occur 3 days after starting therapy and/or in patients with prior heparin treatments.
Low Molecular Weight Heparin (LMWH)
Low Molecular Weight Heparin (LMWH) is another treatment option. Overall, there are advantages of this treatment over continuous heparin infusions. Some of the better benefits for LMWH are better bioavailability, once to twice daily dosing, and less risk of bleeding. Bleeding risk is lower because there is more specific action on factor Xa. LMWH does not require monitoring, and there is also less risk for heparin-induced thrombocytopenia. This medication can also be used in the outpatient setting for first-time uncomplicated DVT in conjunction with starting warfarin.
Warfarin
Warfarin is taken orally for anticoagulation, and it will be started during heparin therapy. Treatment with warfarin usually lasts about 3 months. It stops coagulation by inhibiting the synthesis of vitamin K clotting factors (II, VII, IX, X). Warfarin does take a few days for anticoagulation to be therapeutic, which is why it needs to be started with heparin treatment. There is also a prothrombotic state for the first few days due to inhibition of anticoagulant protein C. INR levels are checked for the therapeutic level, and the levels should be between 2-3. This level needs to be there for at least 24 hours before heparin can be discontinued. This is also a cheaper alternative to the NOACs.
Summary
Deep Venous Thromboembolism and other associated vascular disorders are very common in medicine. An understanding of the cause, diagnosis, and current treatment is essential to safely managing this condition.

References
“Condition-Specific Dosing for Xarelto®.” XARELTO® (Rivaroxaban), 18 Jan. 2022, https://www.xareltohcp.com/dosing-all-indications.
Pai, Menaka, and James D Douketis. “Patient Education: Deep Vein Thrombosis (DVT) (Beyond the Basics).” Edited by Lawrence LK Leung and Geraldine Finlay, UpToDate, 17 Mar. 2022,
“Taking Eliquis.” Taking ELIQUIS® (Apixaban) for DVT/PE Treatment | Safety Info, https://www.eliquis.bmscustomerconnect.com/vte/taking-eliquis.
Rasmussen, Todd E., et al. Handbook of Patient Care in Vascular Diseases. Sixth ed., Wolters Kluwer, 2019.
LEARN MORE ABOUT DVT AND OTHER ACUTE MEDICAL CONDITIONS BY TAKING OUR SELF-STUDY EMERGENCY MEDICINE AND HOSPITALIST COURSES!
