Josh Nowocin, PA-C
Performing a thorough abdominal examination is a core skill every advanced practice provider should know. This exam plays a key role in determining a patients gastrointestinal and/or genitourinary pathology. It can also provide insight into other anatomical abnormalities. A detailed and thorough abdominal exam also decreases the need for radiologic testing. It allows the provider to focus on the patient’s pain management.
General Inspection
The abdominal exam begins with the patient laying supine with arms laying at their side. The provider should expose the abdominal area, ideally from the nipples to the lower abdomen. General inspection can show the presence of different signs that may indicate different disorders. For example, distention of the abdomen could be related to bowel obstruction, tumor/mass, cancer, pregnancy, or other conditions.
Abnormal masses may indicate a hernia, depending on location. A thorough exam can also demonstrate the possibility of tumors. A patch of ecchymosis may be visible on any part of the abdomen which could reflect internal hemorrhage. Ecchymosis of the flank and groin is known as a Grey Turner Sign. This may suggest hemorrhagic pancreatitis. Ecchymosis in the periumbilical area is known as a Cullen sign. This can be seen in patients who have retroperitoneal hemorrhage or intra-abdominal bleeding. The presence of different types of scars may be related to surgery and/or traumatic injuries such as gun shot or stab wounds.
Cushing’s Syndrome may appear as pink-purple striae on the skin. Patients with hepatic cirrhosis can present with Caput Medusae. These appear as distended veins flowing away from the umbilicus. Liver disease can also cause Caput Medusae. You may see these findings with or without jaundice. Post-surgical patients may have a stoma present or could also present with a fistula associated with the surgical tract. Performing a thorough abdominal exam helps to ensure you don’t miss these things!
The abdomen can be divided into quadrants that cross at the umbilicus. Likewise this provides four separate quadrants (Right and Left, Upper and Lower). Clinicians will also refer to three common areas as well – Epigastric, Umbilical, and Suprapubic (Hypogastric).
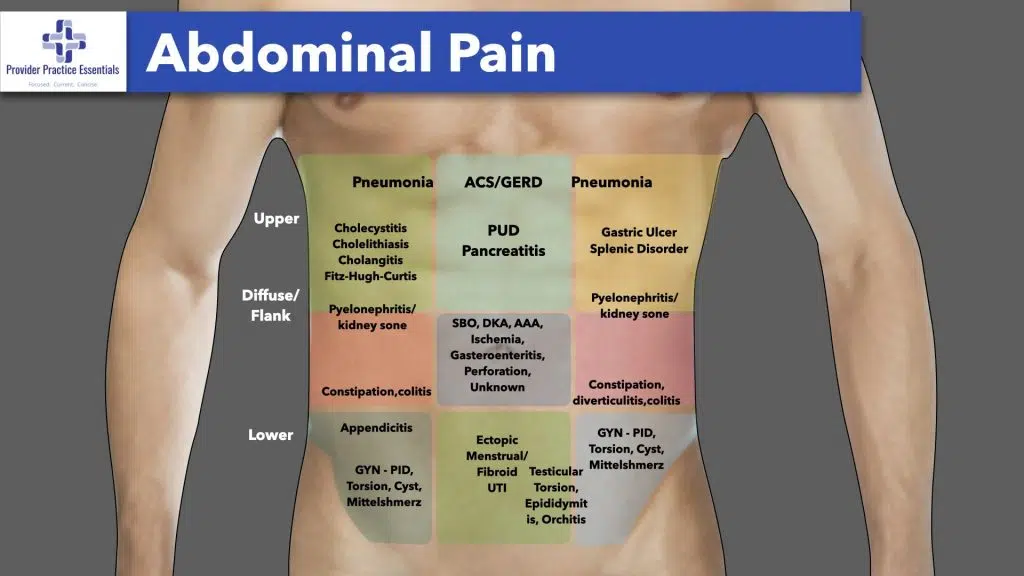
Auscultation
Auscultation is an important part of performing a thorough abdominal exam. Using your stethoscope, gently place the diaphragm over the different quadrants to elicit bowel sounds. Normal bowel sounds are low-pitched and gurgling. The typical rate is usually between 2 and 35 per minute. Listening in one location is typically sufficient. This is because bowel sounds are widely transmitted through the abdomen. However, auscultating in other areas may help localize ones pain with light pressure as well as finding other anomalies like bruits or friction rubs. These sounds are associated with vascular insufficiency. They are also heard with liver or spleen pathology such as infarction or tumors. Likewise, absent bowel sounds may indicate paralytic ileus. Hyperactive rushes (borborygmi = stomach growling) are usually present in small bowel obstruction. This can also be heard in patients with lactose intolerance.
Percussion
Percussion the abdomen will help you determine the amount and distribution of gas in the abdomen. It will also help to identify possible masses that are solid or fluid filled. You can also use percussion to assess the size of the liver and spleen. You should percuss in all four quadrants of the abdomen. A distended abdomen that is also tympanic on percussion suggests an intestinal obstruction. Percussion is also a key component of performing a thorough abdominal exam.
Percussion of Liver and Spleen
Liver
To determine the upper limits of the liver, begin percussing in the midclavicular line just below the nipple. Percuss down from lung resonance down toward liver dullness. Measure in centimeters the distance between the upper and lower limits of the liver. The normal size of a liver on the right midclavicular line is between 6-12 cm and the midsternal line is 4-8 cm. The liver is larger in men than women.
Spleen
Percuss the left lower anterior chest wall between the lung resonance and the costal margin (Traube’s space). You should also check for a splenic percussion sign. To do this, percuss the lowest interspace in the left anterior axillary line. This area is usually tympanic. Then ask the patient to take a deep breath, and percuss again. When spleen size is normal, the percussion note usually remains tympanic. An enlarged spleen will sound dull to percussion.
Palpation
Before palpating, have the pain point to where their pain is most severe. There are three stages of palpation that include superficial or light palpation, deep palpation, and organ palpation. The entire abdomen should be palpated in a systematic order. Always make sure the patient is in a supine position with hands to their sides. Initially, start with light palpation furthest away from the area the patient has showed you. If no pain, then the practitioner can begin anywhere, but moving systematically through the different quadrants. A provider may be able to palpate crepitus or also note other masses like hernias or lipomas.
Next, you should move toward deep palpation with gentle and steady firm pressure. With palpation over the abdomen, determine whether the patient has voluntary or involuntary guarding. This may be a voluntary process, in which the patient voluntarily tightens the abdominal muscles to protect a deeper inflamed structure, or an involuntary process. In these cases an intra-abdominal pathology has likely progressed to cause rigidity of the abdominal muscles. You should note abdominal tenderness. The different quadrants of the abdomen should elicit further specialized palpation/maneuvers to determine possible diagnosis or imaging studies required.
Right Upper Quadrant
The primary pathology to consider with the right upper quadrant is Acute Cholecystitis. A sharp increase in tenderness with a sudden stop in inspiratory effort constitutes a positive Murphy’s sign. A jagged stone obstructing the biliary system irritates the gallbladder wall and causes pain.
Epigastrium
Common diagnoses in this location include gastritis, pancreatitis, and also acute cholecystitis.
Right Lower Quadrant
Acute appendicitis classically causes right lower quadrant pain. McBurney’s point is located in a mid-diagonal position between the umbilicus and the right inguinal ligament. Tenderness here is also very commonly diagnostic of acute appendicitis. There are other exam techniques to elicit if RLQ tenderness in acute appendicitis.
- Rovsing’s sign: While standing on the patient’s right side, gradually perform deep palpation of the left lower quadrant. Increased pain on the right suggests right sided peritoneal irritation.[3]
- Psoas sign: Place your hand just above the patient’s right knee and ask the patient to push up against your hand. This results in contraction of the psoas muscle which causes pain if there is an underlying inflamed appendix.[3]
- Obturator sign: You can test this by by flexing the patient’s right thigh at the hip with the knee flexed. Rotating internally causes increased pain at the right lower quadrant and suggests inflammation of the internal obturator muscle from overlying appendicitis or an abscess.
- Cutaneous Hyperesthesia: Pick up a skin fold between your thumb and index finger without pinching, this maneuver should not be painful, but localized pain could accompany appendicitis.

Umbilical
Hernias are common in the location, especially in young children. To determine whether a hernia is present, ask the patient to cough or bear down
Left Lower Quadrant
Diverticulitis causes left lower quadrant pain. Other diagnoses to consider while palpating include abdominal and gynecologic causes in females. A mass, if present may be due to a tumor of the colon, a left ovarian cyst, or ectopic pregnancy. Impacted stool and constipation can typically be present in the elderly.
Aorta
Palpation of the aorta should be performed by placing the left and right hands along the lower borders of the left and right costal margins. The examiner’s fingers should point toward the umbilicus. This is to determine if there is a pulsatile mass reflective of an abdominal aneurysm. These patients will likely require additional imaging. An emergency department setting may be most appropriate for these patients.
Digital Rectal Exam
To examine the rectum, place your lubricated, gloved finger against the patient’s rectal sphincter muscle to dilate the sphincter and slowly slide it into the rectum to palpate for hemorrhoids, fissures, or foreign bodies. You should evaluate the prostate for size and also firmness. Any tenderness or bogginess suggests prostatitis, and any nodules may also suggest cancer. You should inspect your finger for signs of active bleeding or melena. A Hemoccult test should be performed. The external genitalia should also be examined at this time.
Summary
Although the differential diagnosis for abdominal pain can be broad, a consistent, reproducible examination is the single best tool a provider can have to identify disease. Performing a thorough abdominal exam should become part of your normal patient encounter. It is my hope that this process will help you help your patients!
RESOURCES:
- Bates Guide to Physical Exam – Bates_guide_to_physical_examination_MCQs.pdf (ucoz.net)
- Abdominal Exam – StatPearls – NCBI Bookshelf (nih.gov)
- Snyder MJ, Guthrie M, Cagle S. Acute Appendicitis: Efficient Diagnosis and Management. Am Fam Physician. 2018 Jul 01;98(1):25-33.
If you found this article helpful, you should check out our clinical toolkit!
